10 Best Orthopedic Implant Fixation Techniques Explained
Orthopedic implant fixation plays a critical role in modern orthopedic surgery. This technique ensures that implants, such as plates, screws, and rods, remain securely attached to bones during the healing process. Proper fixation is vital for successful recovery and improved patient outcomes.
Surgeons must consider various factors when selecting an appropriate fixation technique. These factors include the type of fracture, location, and the patient’s individual needs. Each method has its advantages and limitations. Understanding these differences is essential for optimizing surgical success.
New advancements continue to emerge in orthopedic implant fixation. These innovations aim to enhance stability and reduce complications. However, even the best techniques may not guarantee perfect results. Continuous learning and adaptation are necessary in this ever-evolving field. Each case provides a unique challenge, and reflection on past outcomes can lead to improved practices.
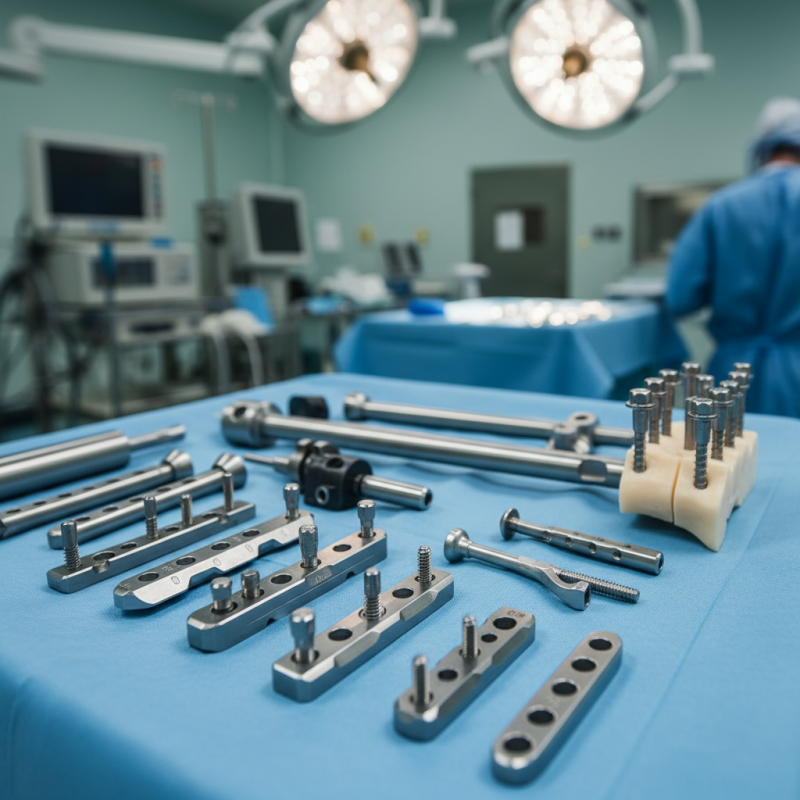
Overview of Orthopedic Implants and Fixation Techniques
Orthopedic implants play a critical role in modern medicine, aiding surgical procedures to repair bones. They help stabilize fractures, correct deformities, and replace damaged joints. These implants include screws, plates, rods, and bioresorbable materials. According to a report by the Global Orthopedic Implants Market, the sector is expected to reach over $60 billion by 2026, reflecting significant advancements and demand for innovative fixation techniques.
Fixation techniques are crucial for the effectiveness of implants. Traditional methods include internal fixation, using metal screws and plates, and external fixation, which provides stability from outside the body. However, each technique has its challenges. For instance, while internal fixation offers strong strength, it can lead to complications, such as infection or implant failure. The choice of technique often depends on the type and location of the injury, patient age, and overall health.
Emerging techniques, like minimally invasive surgeries and 3D-printed implants, present new opportunities. They promise reduced recovery times and improved outcomes. Yet, they also require extensive training for surgeons and carry risks of complications. Continuous evaluations and feedback loops are essential to refine these methods and ensure patient safety. Balancing innovation with proven practices remains a critical focus for the orthopedic community.
Understanding Bone Healing and the Role of Fixation
Bone healing is a complex process, crucial for recovery after orthopedic procedures. Fixation techniques play a significant role in stabilizing fractures, promoting proper alignment, and enabling natural healing. Clinical studies show that optimal fixation can reduce healing time by up to 30%. According to the Journal of Orthopedic Research, proper fixation is essential for lower rates of complications and improved patient outcomes.
Effective fixation techniques include intramedullary nailing and plate-screw systems. These methods provide stability and allow for early mobilization. Recent research indicates that patients who engage in early movement are 50% more likely to report satisfaction post-surgery. However, not all fixation methods suit every type of fracture. Each case requires a thorough assessment by a qualified orthopedic surgeon.
When considering fixation options, here are a few tips:
- Communicate openly with your healthcare team. Understanding your specific fracture and treatment plan is vital.
- Follow post-operative instructions strictly. Compliance can significantly enhance healing rates.
- Consider rehabilitation as part of the healing process. Engaging in physical therapy under expert guidance can improve recovery.
Common Types of Orthopedic Implant Fixation Techniques
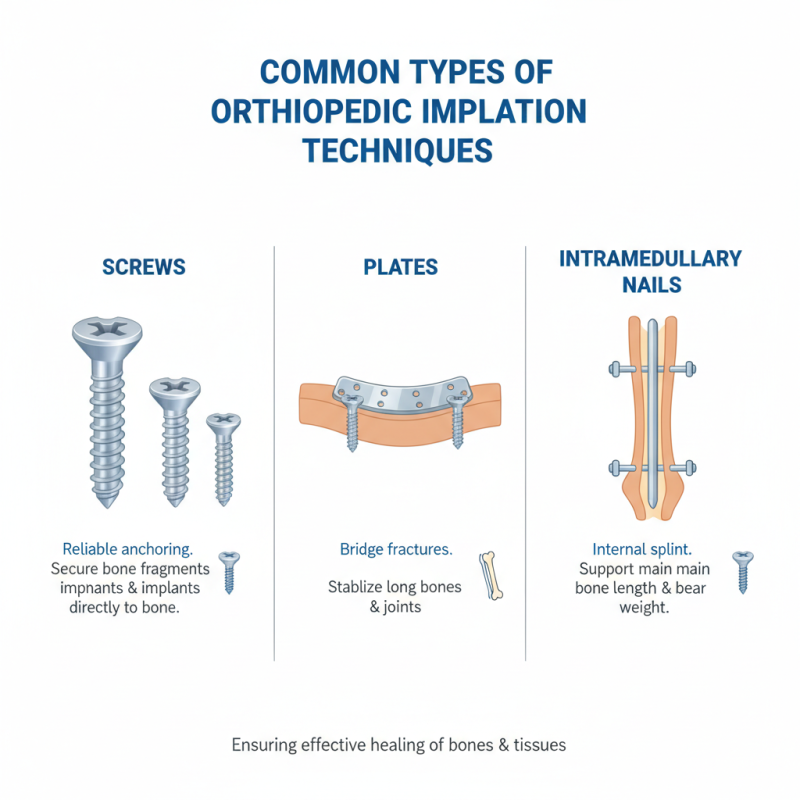
Orthopedic implant fixation techniques are vital in ensuring effective healing of bones and tissues. Common types include screws, plates, and intramedullary nails. Each technique serves a unique purpose in stabilizing fractures and joint replacements. Screws offer reliable anchoring for bone fragments. They come in various types like cancellous and cortical screws. These screws help secure implants directly to the bone.
Plates serve as an external support, particularly in complex fractures. They distribute stress along the bone, promoting stability. Different plate designs cater to specific injury types. Intramedullary nails insert into the medullary canal of bones, providing internal support. This technique is less invasive and can shorten recovery time.
Despite advancements, challenges exist in implant fixation. Inadequate fixation can lead to complications like non-union fractures. Surgeons must weigh the pros and cons of each method carefully. They need to be aware of the unique needs of each patient. Learning from past experiences helps refine technique choices. Understanding these fixation methods allows for improved patient outcomes. Reliable techniques are essential for successful recovery pathways.
Step-by-Step Guide to Each Fixation Technique
When considering orthopedic implant fixation techniques, it’s crucial to understand each method's intricacies. Start with plate fixation, which involves securing the implant to the bone using screws. The alignment of the plate must be precise to ensure optimal stability. Surgeons often face challenges with this technique, especially in complex fractures.
Next, consider intramedullary nailing. This technique uses a metal rod inserted into the marrow canal of the bone. While it can provide excellent support, achieving the correct length and angle is complex. Misalignment can lead to complications, making careful planning essential.
External fixation is another option. It involves stabilizing the bone from outside the body with pins and rods. This method is useful in cases of severe fractures or infections. However, it requires ongoing care and monitoring to avoid issues with the pins. Each technique comes with its challenges, emphasizing the need for thorough understanding and experience in selecting the right method for specific cases.
Orthopedic Implant Fixation Techniques - Comparison of Effectiveness
Recent Advances and Innovations in Implant Fixation Methods
Recent innovations in orthopedic implant fixation have significantly enhanced outcomes in surgical procedures. New materials, such as bioresorbable polymers, are being utilized to create implants that can dissolve over time. This reduces the need for a second surgery to remove the implant. According to a 2022 study, bioresorbable implants showed a 30% improvement in healing time for certain fractures compared to traditional titanium options.
Robotic-assisted surgery is also becoming more prevalent. Reports indicate that this technology can increase precision in implant placement by 15% to 20%, leading to better alignment and fewer complications. Surgeons are adopting these techniques at a rapid pace, but challenges remain. Training and integrating this advanced technology into surgical practice can be daunting. Some surgeons express concerns about the steep learning curve and the potential for technical failures during operations.
Another promising advance is the use of 3D printing for custom implants. This method allows for patient-specific designs that fit perfectly within the anatomy. A recent survey revealed that 82% of orthopedic surgeons believe 3D-printed implants provide better patient outcomes. While these advancements provide exciting possibilities, the industry must address issues related to cost and accessibility, ensuring that all patients benefit equally from these innovations.
Related Posts
-

2026 Top Trends in Orthopedic Surgical Outcomes You Need to Know?
-
China Top Knee Implant Technology Advancements and Innovations?
-
How to Choose the Right Orthopedic Implant Fixation Method?
-
Joint Pain Treatment Options Every Buyer Needs to Know?
-
Top 10 Advanced Joint Implants Transforming Orthopedic Surgery?
-

Top Strategies for Orthopedic Mobility Restoration Techniques?
Copyright © 2021 United Orthopedic Corporation All Rights Reserved.